Most GPs are feeling at least somewhat confident with telehealth technology, and just over half have done a telehealth consultation by video at least once in the COVID-19 pandemic.
Welcome to The Medical Republic‘s COVID Catch-Up.
It’s the day’s COVID-19 news into one convenient post. Got any tips, comments or feedback? Email me at bianca@biancanogrady.com.
6 August
- Most GPs confident with telehealth and plan to continue if item numbers extended, RACGP survey finds.
- General practices in Victoria stay open, but must have a COVID Safe Plan.
- Attacks on public health officials in the US during COVID-19 pandemic leading to resignations.
- Sydney’s inner west on notice after COVID-19 case visits multiple venues.
- Most GPs are feeling at least somewhat confident with telehealth technology, and just over half have done a telehealth consultation by video at least once in the COVID-19 pandemic, according to an RACGP survey of 420 members.
The survey found nearly one third of respondents were very confident with telehealth technology, and the majority of those surveyed said they would continue to use telehealth to provide care if the temporary MBS item numbers were extended beyond September.
Telehealth was also popular with patients, with one in five GPs reporting that 61%-80% of their patients have asked for telehealth.
Telephone consultations were much more popular than video, with 97% of respondents having done phone consultations. The most common reasons for choosing telephone over video were either that the video would not have offered any benefits beyond a phone call, or that the hardware or software for video calls wasn’t available.
However 65% of those not using video said they’d be happy to use it if the patient requested it, if the technology was available to them, or if there was better remuneration for video telehealth.
Among those who did use video, around one-quarter said it helped them to assess the patient, 19% said it helped them to do a physical examination of the patient, and 19% also said they found it to be more personal.
The most popular platforms used for video consultations were FaceTime, Zoom and Skype, used on a personal mobile device, practice computer or personal computer. - While general practices are on the list of workplaces that are permitted to stay open during the stage 4 restrictions in Melbourne, that means they are also required to have a COVID Safe Plan. If your practice doesn’t already have one, the Victorian health department has provided guidance on creating one.
- There is no situation that trollish idiots can’t make worse by being trollish idiots. In the US, there are increasing reports of attacks on health officers, including doxing (publishing their private information such as contact details), armed protests at their homes, vandalism, harassment and threats via social media.
According to a report in JAMA, 27 health officials in 13 states have either resigned or been fired since the start of the pandemic. “It reflects misunderstanding of the pandemic, biases in human risk perception, and a general decline in public civility,” the article’s authors wrote. They warned that “without protection and support, the already scarce supply of qualified individuals willing to serve in health officer roles will decline further.” - Sydney’s inner west is on alert after a man who later tested positive for COVID-19 dined at the Jambo Jambo African restaurant in Glebe on 31 July from 7pm to 8.30pm, then visited several other venues over the next two days including the Eveleigh Hotel in Redfern, Warren View Hotel in Enmore, three venues in the CBD, and Marrickville Woolworths. Anyone who visited these venues around the 1 and 2 August should monitor for symptoms, and if they occur, self-isolate and get tested immediately.
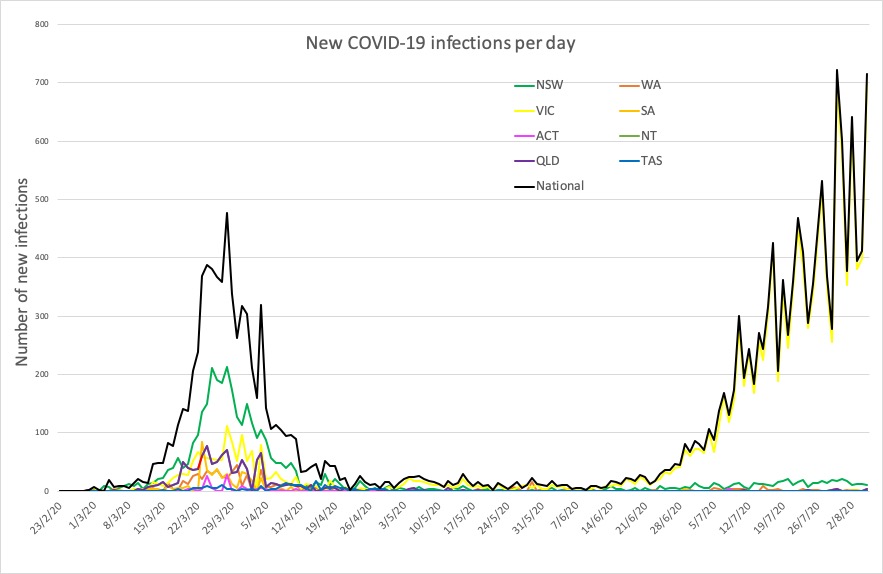
Here are the latest confirmed COVID-19 infections numbers around Australia to 9pm Wednesday:
National – 19444, with 247 deaths and 566 hospitalised.
ACT – 113
NSW – 3820
NT – 33
QLD – 1088
SA – 456
TAS – 229
VIC – 13,035
WA – 670