Burnout is a late-stage reaction to chronic stress, an Australian researcher says.
GPs who work at least 50 hours a week or who don’t feel a sense of autonomy at work are more likely to experience burnout, but are less likely to feel burnt out if they have weekend appointments, new research shows.
The findings come as an Australian researcher argues in a new paper that burnout is a late-stage reaction to chronic stress where self-protective psychological mechanisms help protect against further psychological stress.
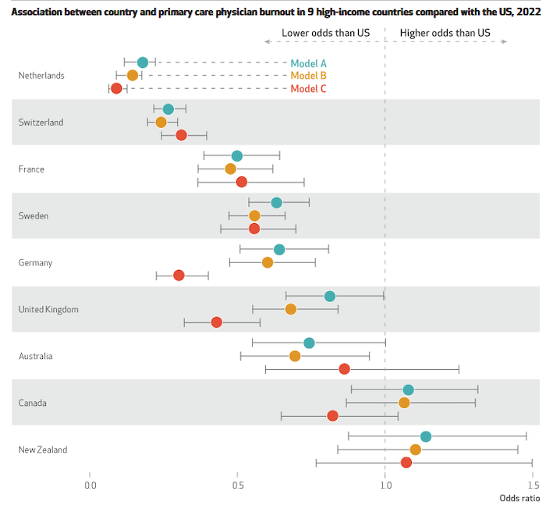
“Primary care physicians remained under stress and at risk for burnout across several high-income countries, including the US,” the researchers said in Health Affairs.
In an analysis of dissatisfaction, stress, and burnout in the US and nine other countries, the US researchers found that female physicians had 31% higher odds of burnout, while physicians who said their workload increased after the pandemic had 41% higher odds.
Doctors also had higher odds of burnout if they worked at least 50 hours a week (37%), had at least 45 consultations a week (35%) and if they thought they provided worse quality of care after the pandemic (84%).
But doctors aged 65 and over had 32% lower odds of burnout, the researchers said.
And in a finding the researchers said was “counterintuitive”, doctors who provided more than two weekend appointments each month were 71% less likely to experience burnout.
“The relationship between providing more weekend appointments and lower burnout odds appears counterintuitive but may reflect a level of scheduling flexibility and autonomy or the fact that primary care physicians experiencing burnout are less likely to offer weekend care,” they said.
“The association between perceived work-life balance and lesser burnout, even after workload is controlled for, underscores the importance of broader cultural and structural supports that enable primary care physicians to manage their roles both within and beyond the workplace.”
In most of the countries included in the study, female primary care physicians were more likely than male GPs to report burnout.
“In addition, female physicians were more likely to experience stress than male physicians across all countries in 2022, although not consistently in earlier survey years.
“These findings are in line with literature suggesting worsened gender inequality in household labour and childcare obligations during the covid-19 pandemic.”
Related
Differences in work patterns between male and female doctors may be to blame for that difference, the researchers said.
“Women receiving more messages from colleagues and patients than men in the setting of increased message volume overall during and post-pandemic, women spending more time with patients per visit, and gendered patient expectations, might also contribute to lasting and increasing sex and gender differences.”
Overall, the degree of professional autonomy plays a key role in burnout, the researchers said, with studies suggesting that a stronger sense of autonomy protects physicians from burnout.
“In the US, poorer control over work has been associated with physician burnout.”
The researchers said policy solutions could focus on ensuring manageable work hours and administrative work, in-person support structures, fair payment, work-life balance, and the opportunity to provide consistent quality of care.
“Quality improvement initiatives and policies that enhance control over schedules and work-home conflicts are possible first steps,” they said.
“At the same time, persistent and growing sex disparities in physician well-being demand dedicated attention.
“Efforts to improve physician burnout must go beyond one-size-fits-all interventions and account for both systemic and demographic drivers of stress and burnout.”
Australian psychologist Dr Shaun Prentice said the prevalence of burnout in the medical profession “appears to have created vagueness about what ‘burnout’ means”.
“Burnout is conceptually distinct from, but related to, depression, stress and vicarious trauma,” he said in a paper published by the Australian Journal of General Practice this month.
Dr Prentice said the core symptoms of burnout were exhaustion, depersonalisation, reduced sense of achievement, heightened affective reactivity, and cognitive and performance problems.
“Burnout is a late-stage reaction to chronic stress where self-protective psychological mechanisms are invoked to minimise further psychological and physical strain,” Dr Prentice said.
“Burnout shows a distinct aetiology and symptom profile from depression, stress and vicarious trauma.
“Greater understanding of what burnout is will facilitate earlier recognition and more specific intervention to prevent exacerbation.”





