Screening for ADHD symptoms should be a crucial part of managing severe chronic pain, Japanese researchers say.
ADHD symptoms and severe chronic pain could be linked by anxiety, depression and pain catastrophising, according to new a Japanese study.
The research, published in Scientific Reports, was based on evidence suggesting that there is a shared cognitive-affective pathway involving emotional dysregulation, internalising psychopathology and insomnia as a potential mechanism linking chronic pain and ADHD.
“This research began from everyday clinical experience. In our practice, we frequently encounter patients with chronic pain who do not respond well to conventional treatments. Among these patients, many show characteristics commonly seen in ADHD, such as inattention, hyperactivity or impulsivity, and difficulties with emotional regulation,” said lead author Dr Satoshi Kasahara of the Department of Anaesthesiology and Pain Relief Centre at the University of Tokyo Hospital.
“This led us to consider whether ADHD-related traits might be more common in this population than previously recognized, and whether they could be contributing to the persistence and severity of pain.
“We found that ADHD-related traits were more common in these patients than in the general population, about 2.4 times higher. These traits were also closely linked to pain severity, as well as to psychological factors such as anxiety, depression and negative ways of thinking about pain.”
Researchers recruited 958 individuals aged 20 years and older with persistent chronic pain from 13 different multidisciplinary pain clinics located across Japan. Participants completed a series of surveys related to pain characteristics, ADHD and ASD symptoms and other psychological outcomes.
The median age of participants was 58 years, and 40.6% were male. Only a small proportion (8.4%) reported extremely severe pain (a numerical rating scale score of 9 or 10 on a 0-10 scale, where higher scores indicate more severe pain). Seventeen percent of participants screened positive for ADHD (giving at least four positive responses to six items of the Adult ADHD Self-Report Scale that assess inattention and hyperactivity-impulsivity), while 4.4% screened positive for ASD (i.e., scoring ≥33 on the Autism-Spectrum Quotient).
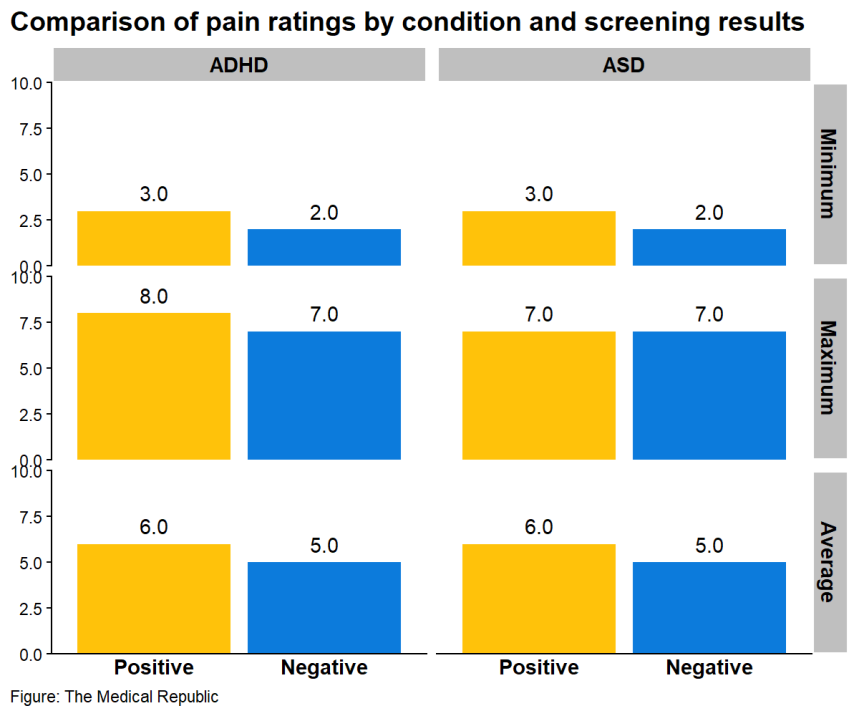
A greater proportion people with extremely severe pain also screened positive for ADHD compared to people without extremely severe pain (27.4% versus 16.1%), but no such association occurred for ASD and extremely severe pain (8.3% versus 4%). Similarly, the ADHD-positive group reported higher minimum, maximum, and average scores on the pain NRS than ADHD-negative people, but there were no differences on these measures between ASD positive and ASD-negative individuals.
Related
Both ADHD-positive and ASD-positive participants scored worse than their screening-negative counterparts on a range of other psychosocial measures, including functional impairment (as measured by the Pain Disability Assessment Scale), insomnia (Athens Insomnia scale), depression and anxiety (Hospital Anxiety and Depression Scale), health-related quality of life (EuroQoL 5-Dimension questionnaire) and pain-related self-efficacy (Pain Self-Efficacy Questionnaire). Only ADHD-positive and ADHD-negative individuals differed on pain-related catastrophic thinking (Pain Catastrophizing Scale).

Further analyses designed to explore the potential associations between ADHD symptoms, mental health, severe chronic pain and other sociodemographic variables were undertaken.
“[These] path analyses suggested that the association between ADHD symptoms and severe chronic pain was explained by indirect pathways mediated by anxiety and depression, either along or in combination with pain catastrophising,” the researchers said.
The findings offer new insights into the potential common mechanisms underlying chronic pain, anxiety, depression and ADHD symptoms.
“Adult ADHD is known to have high comorbidity with depression, anxiety disorders, and insomnia, making it plausible that ADHD symptoms contribute to pain through these associated conditions. However, because clinical diagnoses of ADHD were not established in this study, this pattern should be interpreted as reflecting shared symptom features among ADHD, anxiety, and depression, rather than direct evidence of undiagnosed ADHD,” the researchers said.
A key limitation of the study was that ADHD and ASD symptoms were self-reported, rather than assessed in a formal psychiatric setting.
“However, given the ASRS’s reported false-negative rate of 31.3%, the true proportion of participants who might meet diagnostic criteria for adult ADHD could theoretically be higher than the observed screening positivity. Considering this false-negative rate, an estimated 24.9% of all participants in this study, and 39.9% of those with an average pain score of 9–10 on the NRS, could potentially meet the diagnostic threshold if assessed through a full clinical interview,” said the researchers.
The researchers concluded that detecting and treating ADHD in people with chronic pain may lead to broader health benefits.
“Given that ADHD medications can improve both chronic pain and associated cognitive dysfunction in individuals with comorbid ADHD, the screening and management of ADHD symptoms should be considered a priority in the clinical care of individuals with persistent chronic pain despite standard care,” they wrote.