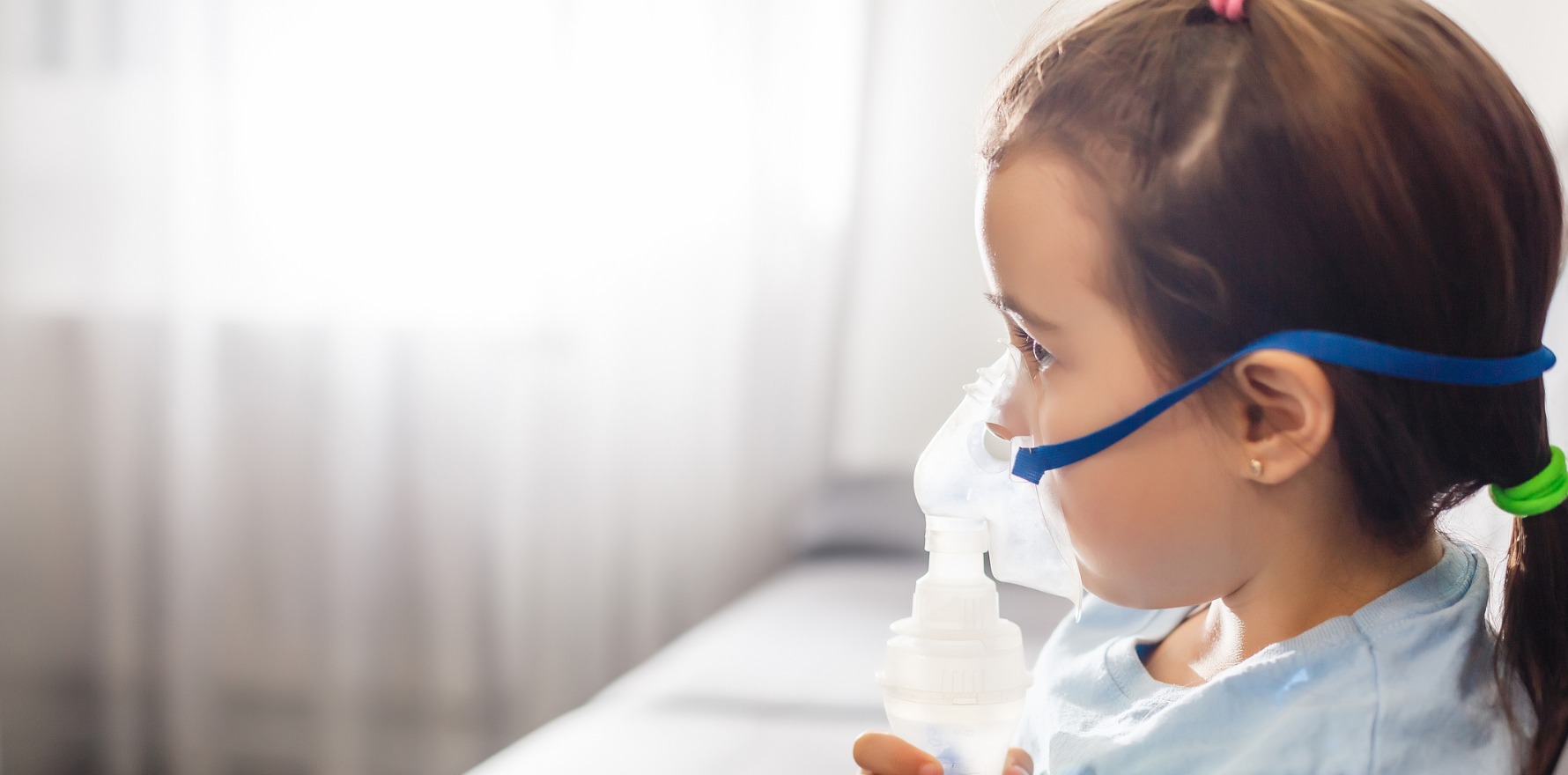
Children are far less likely to be hospitalised for asthma if several easy interventions are made.
ED presentations for kids with asthma have dropped as much as 80% when hospitals have coordinated care with their GP, developed an asthma action plan, and educated children and their carers on the condition, researchers have found.
Now, a growing body of research has backed this as the standard of care in managing children with repeated emergency department visits for asthma attacks.
Dr Nusrat Homaira, senior lecturer in paediatrics at UNSW and respiratory researcher at the Sydney Children’s Hospital, and her colleagues undertook a systematic review and meta-analysis of almost 200,000 children with asthma, and found that community-based interventions could lead to fewer symptoms, sick days from school and less use of health services.
Self-management asthma education, home environmental risk assessment and care coordination were the basis of almost all the community-based interventions studied.
Asthma can’t be fixed in a hospital visit, so Dr Homaira and colleagues were keen to evaluate the usefulness of interventions that addressed the social, behavioural and physiological factors contributing to the disease.
The chief way of doing this was by improving the link between community and hospital asthma services. This research emerged out of previous research undertaken by Dr Homaira and colleagues into care coordination for children with asthma who were frequently presented to hospital.
“Most of these unscheduled asthma presentations can be prevented by ongoing care and regular follow-up,” she said. The 5-10% of children with complex or hard-to-treat asthma were different, but the “vast majority” were manageable, she told TMR.
In 2017, the team collated data on children who had frequent asthma presentations at Sydney Children’s Hospital in Randwick and took participants under the management of a care coordinator. This dedicated staff member ensured children went for a follow-up with their primary care providers after leaving hospital, and sent a letter to the doctor mentioning the hospital presentation.
These children and parents, who also received an asthma action plan and asthma education, had a subsequent 60-80% reduction in emergency department visits.
Thanks to its success, this model became the standard of care in the hospital.
Following this, Dr Homaira and colleagues surveyed hospitals where there were five or more paediatric deaths due to asthma, to understand what follow-up looked like for patients after leaving the hospital.
“We found out from that survey that it was very heterogeneous,” Dr Homaira said. “Every hospital had different things – different asthma action plans were used in different hospitals, different discharge instructions were used in different hospitals.”
That prompted this latest systematic review and meta-analysis, which told the team that a comprehensive community-based model of care had multiple components, including: care coordination, whereby a care coordinator links the children family with their primary care provider; asthma education for children with asthma and their parents; and home assessment of environmental triggers.
“These core components can actually reduce ED presentations, and asthma hospital admissions by 80% in children,” Dr Homaira said. “For every 14 days, the reduction in asthma, daily symptoms and night symptoms reduced by two to three days.”
Those interventions also reduced the need for bronchodilators and improved lung function in some studies.
The team was now implementing this model of care in Liverpool Hospital in South Western Sydney, where children would be randomly assigned to either normal care or management with this suite of interventions.
Children and their parents would get education information, text message reminders to have their regular GP follow-up every three months and an individualised asthma action plan. The team would also provide personal home visits, possibly via technologies such as Skype or WhatsApp, to assess the child’s environment for possible allergens such as poor ventilation, tobacco smoke or pests.
Dr Homaira and her colleagues had not yet analysed the costs of these interventions, but she noted that these services were mostly already available within hospitals – just not necessarily coordinated or used widely.
Beyond savings to the healthcare system, reducing ED visits also saved parents time and money from missing work, not to mention the emotional and psychological stress to the parents and children associated with each asthma attack.
Dr Homaira emphasised the importance of GPs seeing these patients every two or three months in light of the dynamic nature of the condition.