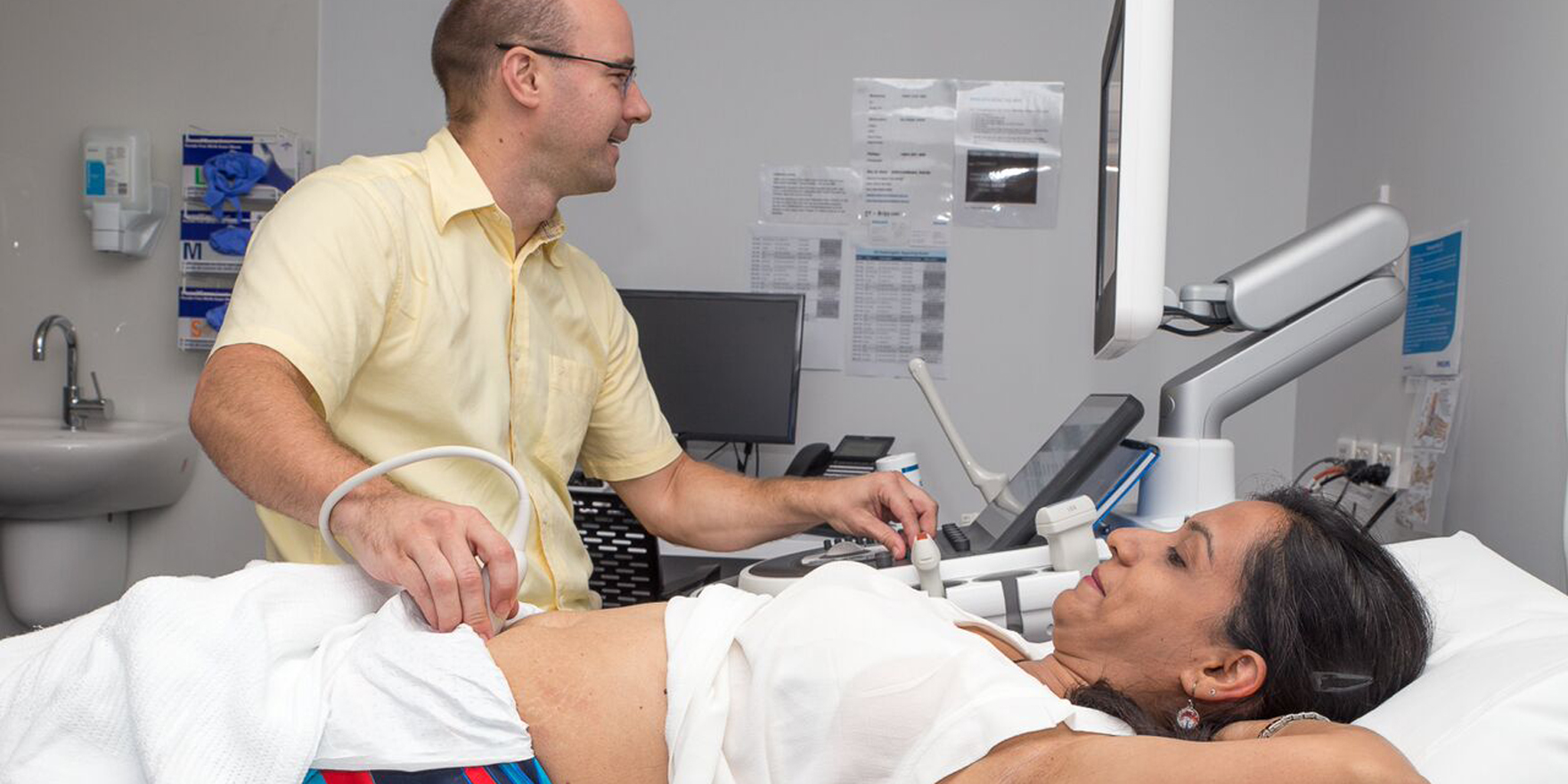
New emergency clinic plans to provide almost immediate care for people with acute conditions, but it comes at a cost
Doctors behind the launch of a walk-in emergency clinic hope to provide almost immediate care for people with acute but non-life threatening conditions, reducing the burden on nearby emergency departments.
Patients visiting the Walk-in Specialist Emergency clinic, located in northern Sydney, will pay a $200 fee that covers consultation with a senior emergency physician, treatment and diagnostic imaging.
The clinic, which launches today, and is equipped with a CT scanner, X-ray OPG, ultrasound and pathology laboratory to further reduce wait times.
Dr Pankaj Arora, an emergency physician at Royal North Shore Hospital and one of the clinic’s founders, pointed to figures showing more than two in three patients who visited the emergency department leave without being hospitalised.
This indicated a need for an in-between service, that treated conditions beyond those normally covered in general practice, such as heavy concussions, fractures and lacerations, but would not necessarily need hospitalisation, he said.
Dr Arora and his colleagues anticipate that around half of the presentations will come from GP referrals, with the other half mainly accounted for by the clinic’s extended opening hours of 10am to 10pm.
The triage system was simple, Dr Arora explained: “If you are looking sick just go in to see a doctor, or if you are looking well then sit here in the reception”.
“We want only 40 to 50 patients here per day, but we will be geared up to take them straight in,” he said.
If patients arrive in need of urgent hospitalisation, or deteriorate while in care, the clinic has an ambulance bay to help get them to a nearby hospital.
The permanent staff includes around 15 emergency physicians, all of whom will continue to work part-time elsewhere to ensure their skillset is maintained.
The clinic also includes several consultation rooms for specialists such as orthopaedicians, obstetricians and dentists.
So rather than being sent out into the community to organise their own care, patients can return to the clinic to see a specialist, and their GP is notified with a report on the patient’s condition.
RACGP president Dr Bastian Seidel welcomed the clinic’s commitment to communicating with the patient’s general practitioner, but said he was unsure if there was a need for walk-in presentations.
“The first port of call for patients should always be to a general practitioner, who is trained in acute presentations, and to take it from there,” he said.
While it was ultimately the patient’s choice whether to pay the out-of-pocket fee, Dr Seidel said there was some concern already that patients were already being over-investigated with technologies such as CT scans, X-rays, ultrasounds and pathology.
“My concern is that a presentation there may potentially lead to lots of follow-up investigations, that would of course attract a Medicare rebate and be a cost to the taxpayer,” he said.
While variations on this model have been widely rolled out across the US, this is one of Australia’s first such clinics.
Patients returning to the clinic within 24 hours are covered by the initial $200 fee, and pay an extra $100 for any other consultations made within a week of the first visit. After that they are subject to another $200 fee.