A pair of recent studies have reinforced the safety and benefits of maternal vaccination during pregnancy for both mother and child.
In the years since the covid pandemic there have been many conversations about the safety and effectiveness of maternal vaccination for various infectious diseases.
Now, two separate studies show that maternal vaccination against influenza, pertussis and covid is not associated with adverse outcomes and protect infants against disease and disease-related hospitalisations.
First, new Australian research has found that concomitant (i.e., same day) vaccination against influenza and pertussis during pregnancy does not result in adverse pregnancy, birth or neonatal outcomes compared to receiving the pertussis vaccine alone.
“Theoretical concerns regarding concomitant administration would include the potential for increased systemic reactogenicity generated in response to vaccination, including fever, leading to adverse outcomes. However, the findings from this study and others suggest this is not the case,” the researchers wrote in JAMA Network Open.
Researchers used data from the NSW Perinatal Data Collection surveillance system and the Australian Immunisation Register to determine whether the rates of pregnancy, birth and neonatal outcomes in women receiving concomitant influenza- and pertussis-containing vaccines differed from women who only received the pertussis vaccine.
There were 6959 women aged 12 to 54 with singleton pregnancies that ended at 20 weeks or later who had concomitant administration of the influenza and pertussis vaccines included in the primary analysis. These women were matched with an equal number of women who received either the pertussis vaccine only or who received both vaccinations on separate days with respect to vaccination date (within 14 days), gestation at vaccination (within one week) and maternal age (within three years).
Women who received their vaccinations prior to 20 weeks of gestation were excluded from the current study. Socioeconomic status, smoking status, covid vaccination status and a previous history of the specific outcome were controlled for in all analyses, along with vaccination date, gestation at vaccination and age.
No differences were observed for the three primary outcomes between women who did and did not receive concomitant vaccination: preterm birth (3.8% versus 4.4%, adjusted hazard ratio and 95% confidence interval 0.83 [0.66-1.05]), small for gestational age (8.8% versus 9.9%, adjusted odds ratio 0.87 [0.74-1.04]) and low birth weight (aOR 0.94 [0.66-1.35]). The researchers had planned to also compare stillbirth rates, but these analyses were not performed due to the small number of events (1.7% across both groups).
A subgroup of 3964 women who received concomitant vaccination and 3964 matched control pregnancies were used to explore additional secondary outcomes. As with the main analysis, there were no differences in the rates or odds of any of the secondary outcomes between concomitant and non-concomitant vaccination groups.
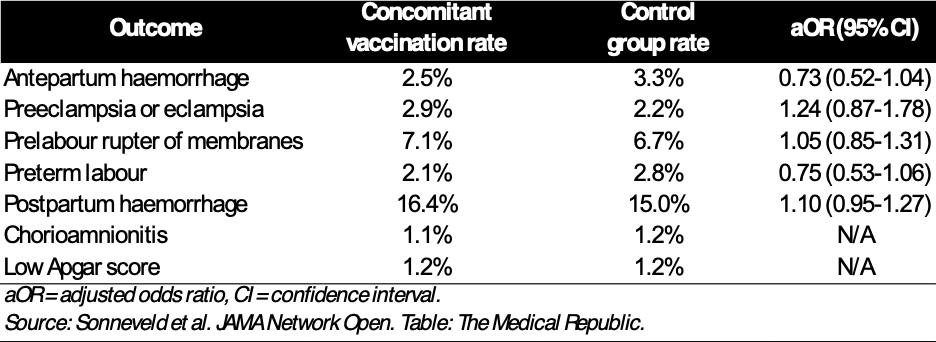
“To our knowledge, this was the first study in which the outcomes of prelabour rupture of membranes, preterm labour, stillbirth, antepartum or postpartum haemorrhage and low Apgar score have been assessed in this context,” said the researchers.
“The evidence presented may help clinicians more confidently recommend pregnancy vaccination concomitantly and potentially provide more opportunities to optimise uptake,” the researchers concluded.
Elsewhere, American researchers have reported that maternal vaccination against covid is protective against infant covid infections and covid-related hospitalisations.
The research, published in Pediatrics, compared the effectiveness of maternal covid vaccination at different stages before and during pregnancy, compared to no vaccination, in preventing covid in infants in the early stages of life.
The single-centre retrospective cohort study involved 78,644 mothers of infants born between July 2021 and June 2023. Infants whose birth mother was younger than 16 years or older than 50 years at the onset of pregnancy were excluded from the current study, as were women who received an mRNA-based covid vaccine less than two weeks before giving birth.
Related
Most women (n = 34,262) were vaccinated during pregnancy or had never been vaccinated (n = 21,087), with decreasing amounts being vaccinated in the three months prior to pregnancy (n = 7930), being vaccinated in the six to 12 months before pregnancy (n = 7268), being vaccinated in the three to six months before pregnancy (n = 6134) or being vaccinated more than 12 months before pregnancy (n = 1963).
There were 3648 infants (4.6% of the total sample) diagnosed with covid during the course of the study, with 943 infants born to unvaccinated mothers, 36 born to women who had been vaccinated more than 12 months before pregnancy, 187 to mothers were vaccinated in the six to 12 months prior to pregnancy, 217 to mothers vaccinated in the three to six months before pregnancy, 404 to mothers vaccinated in the three months prior to pregnancy, and 1861 to women vaccinated during pregnancy.
After adjusting for various maternal factors such as age, ethnicity, parity, BMI, diabetes and hypertension history and socioeconomic status, as well as infant breastfeeding status, the effectiveness of maternal covid vaccination at preventing covid infection in infants under six months (calculated as [1- hazard ratio] x 100) compared to unvaccinated women was 23.6% (95% confidence interval -14.3% to 49.0%) in women vaccinated more than 12 months prepregnancy, 4.5% (-16.8% to 21.9%) in women vaccinated six to 12 months prepregnancy, -3.9% (-24.6% to 13.9%) in women vaccinated three to six months before pregnancy, -14.9% (-32.8% to 0.5%) in women vaccinated less than three months before pregnancy and 7.5% (-2.0% to 16.2%) in women vaccinated during pregnancy.
Vaccine effectiveness for protecting infants from testing positive for covid in the first six months of life was highest when the maternal covid vaccine was delivered in the third trimester when compared to both unvaccinated women (19.2%, 8.6% to 28.6%) and women who were vaccinated prior to falling pregnant (23.8%, 12.1% to 33.9%). There was no association between other timings of the maternal vaccination (i.e., first or second trimester) when comparing to unvaccinated women or women vaccinated before falling pregnant.
Covid-related hospitalisation was confirmed in 76 infants, with 33 infants born to unvaccinated mothers, 18 born to mothers vaccinated before becoming pregnant and 25 born to mothers vaccinated during pregnancy. Vaccine effectiveness for preventing covid-related hospitalisations between birth and six months of age was greatest for women vaccinated during pregnancy compared to unvaccinated women (52.9%, 11.1% to 75.1%) and for women vaccinated during the third trimester compared to unvaccinated women (64.6%, 12.3% to 85.7%).
The researchers concluded that maternal vaccination against covid in the later stages of pregnancy offered the greatest protection against infant cases of covid and covid-related hospitalisations.
“Because infants aged less than six months are too young to be vaccinated themselves and pre-pregnancy maternal vaccination does not appear to be protective, maternal vaccination during pregnancy is likely the most effective way to protect infants against covid,” the US researchers wrote.