The evidence does not necessarily support the government’s oft-repeated refrain.
General practices in Australia are private businesses. They receive payment from patients and the patients then receive a rebate from the Medicare insurance scheme.
The difference between the cost of care and the rebate is commonly called a “gap payment”. If there is no gap payment, the consultation is said to be “bulk billed”.
From a consumer perspective, this looks like “free” general practice consultations.
Some practices, like Aboriginal medical services, state-run primary healthcare services and refugee health services, are funded differently and GPs may be salaried.
In order to provide healthcare “free” to patients, these practices need to draw on funding other than Medicare.
Australians have expressed frustration that general practice is too expensive, and it should be free. There has been pressure from consumers and governments to make general practice “free” for everyone, expecting GPs to bulk bill all consultations.
GPs say bulk billing everyone is impossible to sustain. The Albanese government disagrees.
The policy response
The Albanese government has said that general practice has become too expensive for Australians due to “sustained neglect” of Medicare from previous governments.
Federal health minister Mark Butler has led policy change, increasing investment in general practice by providing incentive payments to general practices that fully bulk bill.
The government has also used a number of other methods to encourage GPs to fully bulk bill, including individual letters to GPs, subsiding certain practices to “intervene in the market” and extensive marketing campaigns to encourage the public to pressure GPs into bulk billing.
It has also funded other “free” services, like urgent care clinics and subsidised primary care services, like pharmacy, to “take the pressure off GPs”, to make “primary care more affordable”.
The evidence
The main source of evidence is from the patient experience survey from the Australian Bureau of Statistics, in which people are asked if they are delaying or avoiding seeing a GP – cost a reason.
At first glance, it seems obvious that the percentage of people avoiding the GP due to cost is increasing, with, perhaps, a decrease as policy initiatives change in 2023-2024.
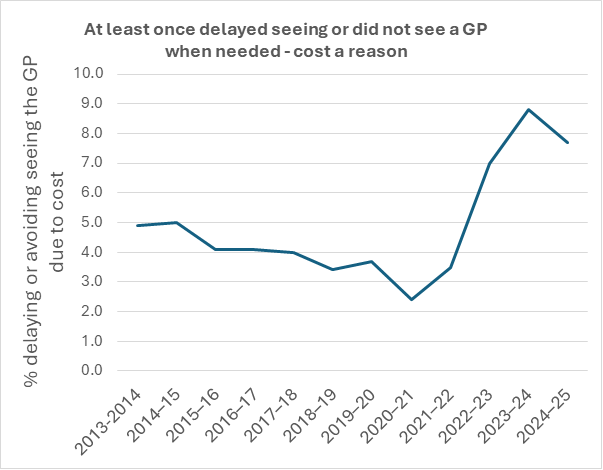
However, the data is more nuanced.
When we examine the data across the socioeconomic spectrum, we see that the richest Australians avoid the GP due to cost almost as much as the poorest.
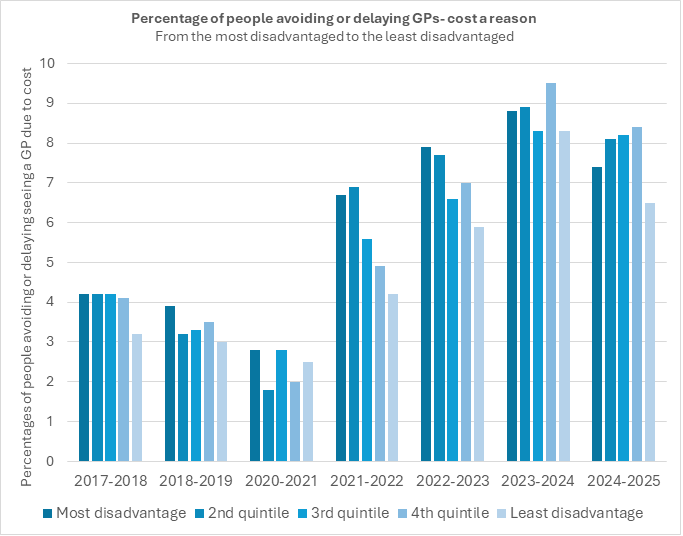
There are a few potential conclusions to be drawn:
- The richest Australians are unlikely to avoid the GP because they can’t afford the gap. It is more likely that they do not choose to invest their money in this service, or that they feel entitled to receive a free service;
- The poorest Australians may be receiving bulk-billed services. Most GPs have mixed-billing practices, bulk billing those with healthcare cards, or with known financial difficulties, while cross-subsiding by privately billing others who can afford to pay;
- Those in the middle socioeconomic groups may well be struggling with multiple financial demands with the increased cost of living.
Less than 10% of Australians avoid the GP due to cost. Some may “avoid or delay seeing the GP – cost a reason” when they can afford to pay, but choose not to.
The impact
GPs are private business owners and contractors who have escalating costs, including rent, insurance, staff and medicolegal costs.
They express considerable frustration over increasing government and public demands, in the face of increasing practice costs. Being expected to bulk bill the rich is impacting the financial wellbeing of GPs, and causing a loss of GPs to general practice, and making general practice less accessible.
The verdict
Less than 10% of Australians are avoiding tor delaying seeing the GP due to cost.
This may well be because some Australians do not choose to pay, rather than being unable to pay.
Entitlement is not poverty.
Subsidising the rich may come at the cost of having a sustainable GP workforce for the whole population in the longer term.
More information
The data can be accessed here. The impact on GPs can be accessed here. The policy approach to affordable primary care can be found here.
Professor Louise Stone is a GP in Canberra and an academic at Adelaide University. A collection of her research, policy and teaching materials can be found at drlouisestone.com.


