Queensland supports whole blood donation assessments that don’t consider sexuality, but Lifeblood prefers the ‘plasma pathway’.
Queensland’s Health Minister has called on the federal government to expedite a new assessment pathway for blood donation that may reduce wait times for some LGBTQIA+ donors.
Currently, men who have sex with men, transgender women and some non-binary people who have sex with men are only allowed to donate blood after abstaining from sex for at least three months.
Over recent years, many countries around the world have scrapped sexual orientation-related rules for blood donation in favour of adopting “individual risk assessments” which ask all potential donors the same set of questions.
But Red Cross Lifeblood – Australia’s government-funded blood donation service – spokesperson Helen Walsh said that if Australia adopted similar assessments, many who were affected by the current rules would still have to wait.
“We know that [the wait period] has been very frustrating for many people and we know there are people in the gay and bisexual community who want to donate,” Ms Walsh told The Medical Republic.
But for those affected by the rules around sexual activity, introducing an individual risk assessment approach for donation – similar to those used by other countries – would only reduce wait times for members of the community in monogamous relationships, said Ms Walsh.
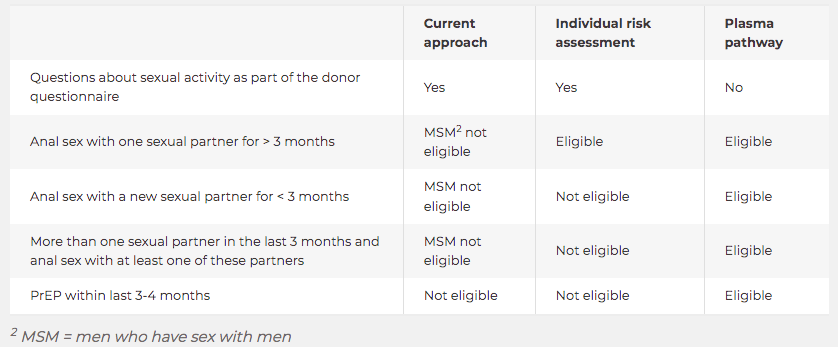
This table from Lifeblood compares three approaches, with individual risk assessment being based on questions used in other countries:
Additionally, according to US research published earlier this year, while almost 60% of the LGBTQIA+ community members surveyed supported individual risk assessments, almost three-quarters believed that the method was still discriminatory, particularly to those using PrEP.
Instead, Lifeblood has been focusing on the “plasma pathway”, which was approved by the TGA earlier this year and would enable anyone to donate plasma regardless of their sexual activity by removing all related questions from the donation questionnaire.
For that to be implemented, CSL Behring – the manufacturer of blood and plasma products – will need to apply for TGA approval for the pathway and states and territories will need to update their questionnaires.
“Plasma is the product most needed by patients and hospitals in Australia and we collect more plasma than blood,” said Ms Walsh.
According to Ms Walsh, implementing the plasma pathway would mean “that if a gay or bisexual man wants to come in to donate tomorrow, but they have had sex with multiple people today, or with a new partner, they would still be eligible to donate plasma”.
Additionally, the plasma pathway would allow individuals on PrEP, who would most likely have “very long wait periods” or would be ineligible to donate under the individual risk assessment approach, to donate plasma.
“There are many gay and bisexual men who are on PrEP to protect their own health and the health of their community,” said Ms Walsh. “They would be able to donate under the plasma pathway.”
She added that although a pathway similar to the plasma pathway could not yet be explored for whole blood as the manufacturing process differs – plasma undergoes fractionation which removes the risk of infection, whereas whole blood is transfused fresh – Lifeblood is still exploring the introduction of individual risk assessments for whole blood.
Advocacy group Let Us Give has pushed back at the plasma pathway saying that it will “entrench a second-class status for gay donors”.
“Plasma-only donation will be to blood donation what civil unions were to marriage equality – a poor substitute for equity and fairness,” said the Let Us Give campaign’s spokesperson, Dr Sharon Dane.
“Assessing each donor for individual risk will maintain the safety of the blood supply while allowing much-needed donations from gay men, as well as bisexual men and trans women who have sex with men,” she said.
Let Us Give said research has shown that individual risk assessments wouldn’t compromise blood safety but would instead increase supply and remove discrimination.
“This is why countries similar to Australia, like Canada, the UK and US have lifted their gay blood bans and adopted individual risk assessment,” said Dr Dane.
Interestingly, data published earlier this year by the Kirby Institute showed that new diagnoses of HIV in the MSM community had halved over the past decade, resulting in Australia’s “world-leading” 10-year decline in HIV cases.
In fact, increasing case numbers have been seen via heterosexual sex – which now accounts for a third of new infections – and among the needle-sharing communities.
In her letter to her federal counterpart Mark Butler, Queensland Health Minister Shannon Fentiman wrote that she “was pleased to see that Lifeblood is removing donor deferrals for plasma donations”.
But she added that “removing barriers for whole blood donations would be a further step in the right direction.”
“We know that many people who could safely donate blood, and who want to help others, are unable to do so under the current rules.
“Obviously, it is critical that we ensure our blood supply is safe for all Australians requiring a transfusion. We have seen individual risk assessment models operate safely and successfully in other countries.
“I look forward to seeing a more inclusive approach to blood donation in the future.”
Ms Walsh said that while Lifeblood will continue “prioritising the plasma pathway because it removes all the wait periods for gay and bisexual men”, it will also continue its research into the individual risk assessment approach for whole blood.





