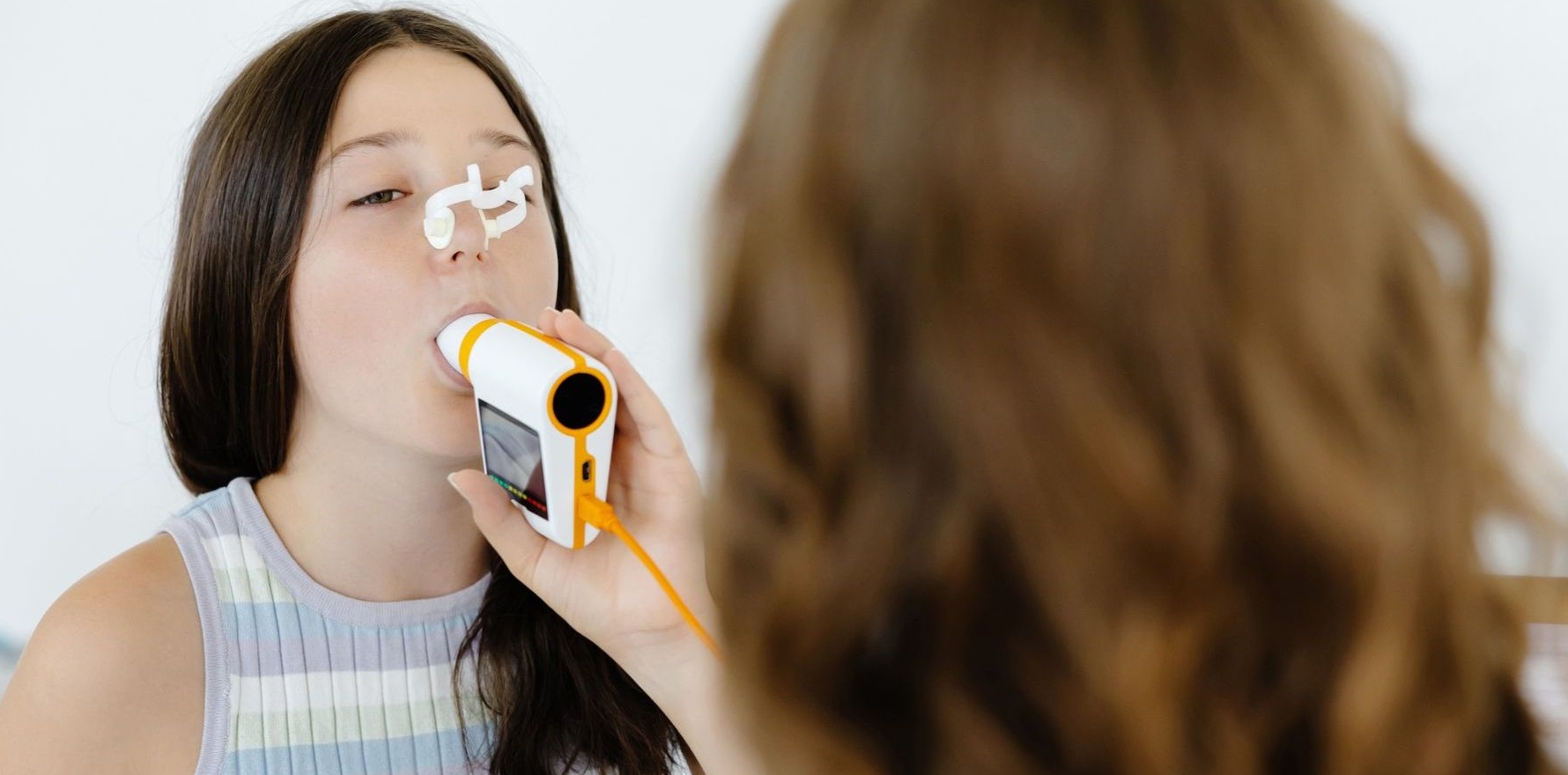
The suite of documents aims to raise quality, consistency and safety of spirometry testing in primary care settings.
Earlier this month the Thoracic Society of Australia and New Zealand released a new set of national spirometry standards.
The standards were developed through a collaboration between national experts and replace the previous TSANZ spirometry standards that were released in 2022. The collection of documents builds on existing international guidelines but are designed to account for the specific needs of Australian primary care settings.
Spirometry is a key part of diagnosing respiratory conditions, but inconsistencies in training, testing quality and interpretation serves as a barrier to accurate diagnoses, especially when the test is performed outside of specialist respiratory laboratories.
Last year Allergy & Respiratory Republic reported that office-based tests for COPD – which are a rough estimate of spirometry use in general practice – had fallen by 78% between 2015-16 and 2022-23. The costs, time, training and infection-control procedures associated with spirometry testing were thought to be responsible for the decline in usage.
Professor Natasha Smallwood, president of TSANZ, said that the decline in spirometry use in primary care had implications for access to timely and accurate diagnosis.
“Spirometry plays a critical role, yet in recent years its use in primary care has become more variable, and in some settings more limited,” she said.
“That variability matters because it affects diagnostic accuracy and the care patients receive. Clear, contemporary standards are essential to support clinicians in delivering high-quality spirometry when it is used in clinical practice.”
The updated standards aim to set “clear national expectations for how spirometry is performed, how competency is recognised and how services can be accredited to deliver reliable, high-quality testing”.
There are three core documents to the new standards.
The first, TSANZ Technical Standards for Spirometry in Australian Primary Care, outlines the key clinical and operational requirements that need to be met to ensure high-quality spirometry can be delivered in a primary care setting in a safe and consistent way.
Related
The second, TSANZ Standards for Training and Maintaining Competency in Spirometry for Australian Primary Care, details the standards that must be met for delivering spirometry training and assessing the competency of individual spirometry operators.
The third, Accreditation Guideline for Spirometry Services in Australian Primary Care, is aimed at organisations and practices that require external spirometry accreditation and outlines the key aspects of the accreditation process, such as equipment, training, procedures and infection control.
There are also plans to release a roadmap for a National Spirometry Program later this year to assist with the longer-term implementation and uptake of spirometry in primary care.
TSANZ CEO Vincent So said the standards being published was an important step, but that supporting their use in everyday practice was the real long-term goal.
“Our aim is to support uptake over time. Equipping clinicians with clear, practical guidance is essential so they can have the confidence and the right tools they need to deliver high-quality spirometry,” they said in a statement.
Funding for the development of the standards was provided by the Commonwealth Department of Health, Disability and Ageing.
Copies of the standards are available from the TSANZ website.