Two dermatologists give tips on how to treat the condition, in the wake of a reported uptick in presentations.
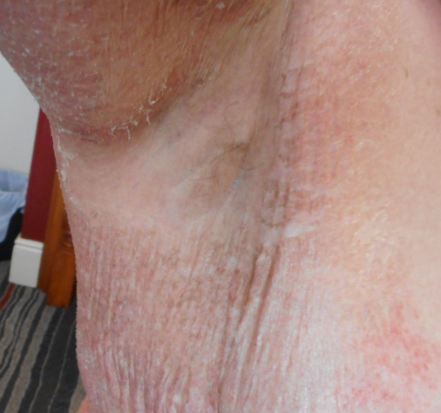
Granular parakeratosis, also known as hyperkeratotic flexural erythema (HKFE), was first described in 19911 as a scaly, pruritic, red-brown macular eruption usually occurring in a symmetrical flexural distribution, especially affecting the inguinal and axillary areas (Figure 1). It was initially described as a possible reaction to deodorant; however, the histology was not consistent with the typical findings in contact dermatitis, and topical corticosteroids did not always help. Non-intertriginous involvement of other areas has also been reported2,3.
Subsequent reports of this condition occurred in the paediatric age group and were linked to the use of benzalkonium chloride (BAK, and sometimes additionally triclosan) in bath oils4,5,6. While the reactions were described as irritant contact dermatitis, atypical features were noted, such as that some cases were not itchy.
Given the particular histological changes, the pathogenesis of granular parakeratosis was hypothesised to be the result of abnormal epidermal differentiation and keratinocyte maturation in the transition between the stratum granulosum and the stratum corneum, resulting in retention hyperkeratosis7. This was believed to be a result of a defect in the production of filaggrin from profilaggrin, resulting in keratohyaline granule retention, and an increased stratum corneum pH, leading to increased adhesion and a defective barrier function8. The lesions were speculated to arise as a protective mechanism; however, chemical irritation was thought to exacerbate this process, especially with occlusion in warm, moist environments with perspiration, skin maceration together with excessive cleaning practices7-9.
This phenomenon was then described with the use of laundry rinses containing BAK in 20172,10. It was subsequently hypothesised that disruption of the skin microbiome from irritants such as BAK might eliminate certain organisms in the skin microbiome, resulting in an environment that allowed other organisms to flourish. However, the causative bacteria were unknown, although staphylococcus aureus, the most common skin pathogen, was thought not to be responsible11.
Granular parakeratosis has been described in patients of all ages12-14 but more commonly affects females15. Some have postulated a link to obesity16. In a case series from New Zealand, 10 of 13 patients were ethnically Asian2.
The role of benzalkonium chloride in laundry rinses and bath oils
BAK is a quaternary ammonium cationic compound widely used as a preservative and antiseptic, and is currently found in many laundry rinses and additives. It is a skin irritant and weak allergen, and has been increasingly implicated in the causation of granular parakeratosis2,10. Clothes contaminated with BAK may contact flexural areas of skin at moisture-rich sites. Anecdotally, there has been an increase in the number of cases of granular parakeratosis presenting to dermatologists in recent times, and we have described a series of 45 cases apparently caused by BAK in laundry rinses17. This has particularly coincided with the covid pandemic, and we hypothesise that anxiety about covid infection have fueled an increased use of laundry antiseptics. Ironically, these have no proven benefit in infection reduction and the SARS-COV- 2 virus is actually sensitive to machine washing in cold temperatures18. The number of people exposed to BAK-containing laundry rinses is unknown, but clearly only a very small proportion go on to develop granular parakeratosis.
How is it diagnosed?
Granular parakeratosis is diagnosed clinically, but there may be a delay in diagnosis if patients do not attend a practitioner familiar with the condition2.
History
Patients usually present with a well-demarcated eruption affecting the flexural or intertriginous areas. Granular parakeratosis has been described as burning and/or painful, and sometimes also pruritic, although may be asymptomatic. Most cases are bilateral; however, reports of unilateral presentations exist1,19. Symptoms may be severe, with marked effects on quality of life, sometimes leading to hospitalisation (R Nixon, personal communication).
The differential diagnosis for granular parakeratosis includes intertrigo, Hailey-Hailey disease (benign familial pemphigus), Darier’s disease, inverse psoriasis, pemphigus vegetans, acanthosis nigricans, confluent reticulated papillomatosis and contact dermatitis. In the paediatric populations, differential diagnoses also include napkin dermatitis, acrodermatitis enteropathica or Letterer-Siwe disease20,21.
Examination
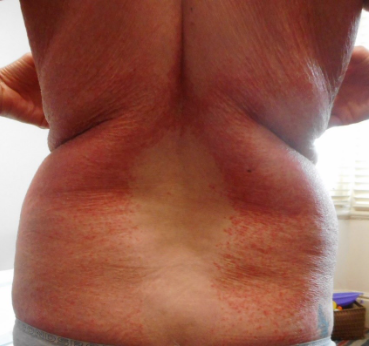
Granular parakeratosis usually presents with red-brown and scaly patches or plaques (Figure 2). It may be discrete, confluent or reticulated with satellite papules14. Less commonly, there may be follicular papules22,23, brown verrucous papules24 or brown macular lesions25.
It usually occurs in the axilla and inguinal areas but involvement of the inframammary folds, abdomen, vulva, penis, perianal area and lumbosacral areas have been reported2,3.
Investigations
The most distinctive histological features of granular parakeratosis comprise keratohyalin granules in the stratum corneum, parakeratosis and epidermal acanthosis7. There may also be capillary dilatation and proliferation in the upper papillary dermis and a scattered perivascular inflammatory lymphohistiocytic infiltrate14. Some findings may overlap with psoriasis2.
Classical histological findings may not always be present and will depend on the stage of evolution of the condition26. For this reason, the condition is usually diagnosed clinically.
The term hyperkeratotic flexural erythema, proposed by Kumarasinghe et al26, is considered by some to be a more appropriate name, given that the term granular parakeratosis refers to histological features that are not always present. They also suggested that patients presenting with clinical features of granular parakeratosis should undergo microbiological evaluation, including skin swabs for bacterial microscopy and culture. All predominant organisms should be reported, even when considered traditional skin flora. Granular parakeratosis has been incidentally linked to tinea and molluscum contagiosum23,27, so fungal cultures may also need to be considered.
As it is likely that granular parakeratosis is a result of skin irritation and not allergy, patch testing to diagnose allergic contact dermatitis is not usually required.
Treatment
Granular parakeratosis is typically recalcitrant to treatment but usually resolves spontaneously eventually.
There is no established treatment pathway for granular parakeratosis, and there is a lack of high-quality studies or trials of treatments. In cases where an irritant is implicated, such as BAK in laundry rinses, it is imperative to recognise the connection, clean the washing machine and rinse clothing repeatedly. However, in many cases disposal of clothing may be required, along with frequent application of a moisturising ointment.
Granular parakeratosis may spontaneously resolve, further blurring the response to treatment.
The use of topical corticosteroids in granular parakeratosis is controversial, with some authors reporting a rapid response to potent topical corticosteroids28,29 whereas others believe they have little use10,11. Woodring et al30 even reported a case of granular parakeratosis associated with the use of the topical corticosteroid triamcinolone.
Other topical treatments reported to be beneficial include salicylic acid31, tacrolimus ointment32 and 40% urea cream33, as well as topical maxacalcitol, a vitamin D3 derivative applied for two months34; topical calcipotriene and ammonium lactate35. Topical calcitriol achieved resolution in 10 days36.
Retinoids, in topical or oral form, have been demonstrated to induce a clinical response in a few cases of granular parakeratosis37,38 with resolution between five days and three weeks. The response to retinoids may relate to their effects on the aberrant cornification process in granular parakeratosis.
The use of amoxicillin-clavulanic acid has been reported to successfully treat granular parakeratosis, with three of the four patients in one case series having no further relapses11. However, a study from New Zealand trialled broad spectrum antibiotic therapy in two patients, with little noticeable improvement2. Our experience included responses to amoxicillin-clavulanic acid, cephalexin and ciprofloxacin in some, but definitely not all, cases.
The use of neurotoxin clostridium botulinum type A has been reported, with resolution of lesions within a few days39, as well as physical treatments such as cryotherapy1, erbium:yttrium-aluminum-garnet (YAG) laser ablation and carbon dioxide lasers40.
Prognosis
Patients with granular parakeratosis may develop secondary bacterial infection, particularly in symptomatic patients with pruritic lesions.
Granular parakeratosis typically resolves in a month to a year14 and appears to be self-limiting. In most cases when BAK is the culprit, cessation of BAK-containing laundry rinses, repeated rinse cycles and occasionally disposal of clothes can lead to resolution of the rash. However, published reports of granular parakeratosis have demonstrated it can persist or chronically recur for up to 20 years41. More research is urgently needed into its pathogenesis and treatment.
Associate Professor Rosemary Nixon and Dr Kajal Patel work at the Occupational Dermatology Research and Education Centre, Skin Health Institute, Carlton, Victoria
References
1. Northcutt AD, Nelson DM, Tschen JA. Axillary granular parakeratosis. J Am Acad Dermatol. 1991;24(4):541-544.
2. Tian CJ, Purvis D, Cheng HS. Granular parakeratosis secondary to benzalkonium chloride exposure from common household laundry rinse aids. N Z Med J. 2021;134(1534):128-142.
3. Delaleu J, Moulonguet I, Breton AL, Bagot M, Fouere S, Dauendorffer JN. Granular parakeratosis involving the glans of the penis and foreskin. J Dermatol. 2020;47(8):e295-e296.
4. Moyle M, Moore EJ, Varigos GA. Characteristic adverse skin reactions to antiseptic bath oils. Med J Aust. 2007;186(12):652-653.
5. Storer E, Koh KJ, Warren L. Severe contact dermatitis as a result of an antiseptic bath oil. Australas J Dermatol. 2004;45(1):73-75.
6. Ling TC, Highet AS. Irritant reactions to an antiseptic bath emollient Journal of Dermatological Treatment. 2000;11(4).
7. Metze D, Rutten A. Granular parakeratosis – a unique acquired disorder of keratinization. J Cutan Pathol. 1999;26(7):339-352.
8. Ding CY, Liu H, Khachemoune A. Granular Parakeratosis: A Comprehensive Review and a Critical Reappraisal. Am J Clin Dermatol. 2015;16(6):495-500.
9. Wohlrab J, Luftl M, Wolter M, Marsch WC. Submammary granular parakeratosis: an acquired punctate hyperkeratosis of exogenic origin. J Am Acad Dermatol. 1999;40(5 Pt 2):813-814.
10. Robinson AJ, Foster RS, Halbert AR, King E, Orchard D. Granular parakeratosis induced by benzalkonium chloride exposure from laundry rinse aids. Australas J Dermatol. 2017;58(3):e138-e140.
11. Kumarasinghe SPW, Chandran V, Raby E, Wood B. Hyperkeratotic flexural erythema responding to amoxicillin-clavulanic acid therapy: Report of four cases. Australas J Dermatol. 2019;60(4):311-314.
12. Wallace CA, Pichardo RO, Yosipovitch G, Hancox J, Sangueza OP. Granular parakeratosis: a case report and literature review. J Cutan Pathol. 2003;30(5):332-335.
13. Braun-Falco M, Laaff H. Granular parakeratosis–a clinical-pathological correlation of 10 cases. J Dtsch Dermatol Ges. 2009;7(4):340-344.
14. Scheinfeld NS, Mones J. Granular parakeratosis: pathologic and clinical correlation of 18 cases of granular parakeratosis. J Am Acad Dermatol. 2005;52(5):863-867.
15. English JC, 3rd, Derdeyn AS, Wilson WM, Patterson JW. Axillary granular parakeratosis. J Cutan Med Surg. 2003;7(4):330-332.
16. Gaul M, Bass J, Wikas S. Granular parakeratosis. Cutis. 2020;105(6):E42-E43.
17. Dear K, Ronaldson C, Gan D, Stavrkoglou A, Nixon R. Hyperkeratotic flexural erythema (more commonly known as granular parakeratosis) caused by benzalkonium chloride in laundry rinses – a cases series and postulation of aetiology. In. Unpublished work
18. Abney SE, Ijaz MK, McKinney J, Gerba CP. Laundry Hygiene and Odor Control: State of the Science. Appl Environ Microbiol. 2021;87(14):e0300220.
19. Ezra N, Karunasiri D, Chiu MW. Unilateral pruritic axillary rash: axillary granular parakeratosis. Arch Dermatol. 2008;144(12):1651.
20. Pimentel DR, Michalany N, Morgado de Abreu MA, Petlik B, Mota de Avelar Alchorne M. Granular parakeratosis in children: case report and review of the literature. Pediatr Dermatol. 2003;20(3):215-220.
21. Patrizi A, Neri I, Misciali C, Fanti PA. Granular parakeratosis: four paediatric cases. Br J Dermatol. 2002;147(5):1003-1006.
22. Joshi R, Taneja A. Granular parakeratosis presenting with facial keratotic papules. Indian J Dermatol Venereol Leprol. 2008;74(1):53-55.
23. Resnik KS, DiLeonardo M. Follicular granular parakeratosis. Am J Dermatopathol. 2003;25(5):428-429.
24. Yang JH, Lee HM, Noh TK, et al. Granular parakeratosis of eccrine ostia. Ann Dermatol. 2012;24(2):203-205.
25. Burford C. Granular parakeratosis of multiple intertriginous areas. Australas J Dermatol. 2008;49(1):35-38.
26. Kumarasinghe SP, Chandran V, Raby E, Wood B. Granular parakeratosis is a reaction pattern in hyperkeratotic flexural erythema. Australas J Dermatol. 2020;61(2):159-160.
27. Pock L, Cermakova A, Zipfelova J, Hercogova J. Incidental granular parakeratosis associated with molluscum contagiosum. Am J Dermatopathol. 2005;27(3):255-257.
28. Chamberlain AJ, Tam MM. Intertriginous granular parakeratosis responsive to potent topical corticosteroids. Clin Exp Dermatol. 2003;28(1):50-52.
29. Channual J, Fife DJ, Wu JJ. Axillary granular parakeratosis. Cutis. 2013;92(2):61, 65-66.
30. Woodring T, Peoria SB, Bradley L, Kentosh J. Granular parakeratosis associated with topical triamcinolone: Case report and literature review Paper presented at: American Academy of Dermatology Annual Meeting 2018 2018.
31. Giraldi S, Abagge KT, Carvalho V. Granular parakeratosis: a report of six cases in children. An Bras Dermatol. 2006;81:59-64.
32. Baum B, Skopit S. Granular parakeratosis treatment with tacrolimus 0.1% ointment: a case presentation and discussion. J Am Osteo Coll Dermatol 2013;26:40-41.
33. Genebriera J, Davis MD, Yang H, Borrowman TA. Papillomatous axillary rash due to granular parakeratosis. J Eur Acad Dermatol Venereol. 2007;21(7):994-995.
34. Demitsu T, Nakamura S, Takazawa M, Kakurai M, Umemoto N, Kawase M. Axillary granular parakeratosis with osmidrosis successfully treated with topical maxacalcitol. J Dermatol. 2019;46(5):e155-e157.
35. Contreras ME, Gottfried LC, Bang RH, Palmer CH. Axillary intertriginous granular parakeratosis responsive to topical calcipotriene and ammonium lactate. Int J Dermatol. 2003;42(5):382-383.
36. Patel U, Patel T, Skinner RB, Jr. Resolution of granular parakeratosis with topical calcitriol. Arch Dermatol. 2011;147(8):997-998.
37. Brown SK, Heilman ER. Granular parakeratosis: resolution with topical tretinoin. J Am Acad Dermatol. 2002;47(5 Suppl):S279-280.
38. Webster CG, Resnik KS, Webster GF. Axillary granular parakeratosis: response to isotretinoin. J Am Acad Dermatol. 1997;37(5 Pt 1):789-790.
39. Ravitskiy L, Heymann WR. Botulinum toxin-induced resolution of axillary granular parakeratosis. Skinmed. 2005;4(2):118-120.
40. Laimer M, Emberger M, Brunasso AM, Ahlgrimm-Siess V, Massone C. Laser for the treatment of granular parakeratosis. Dermatol Surg. 2009;35(2):297-300.
41. Reddy IS, Swarnalata G, Mody T. Intertriginous granular parakeratosis persisting for 20 years. Indian J Dermatol Venereol Leprol. 2008;74(4):405-407.



