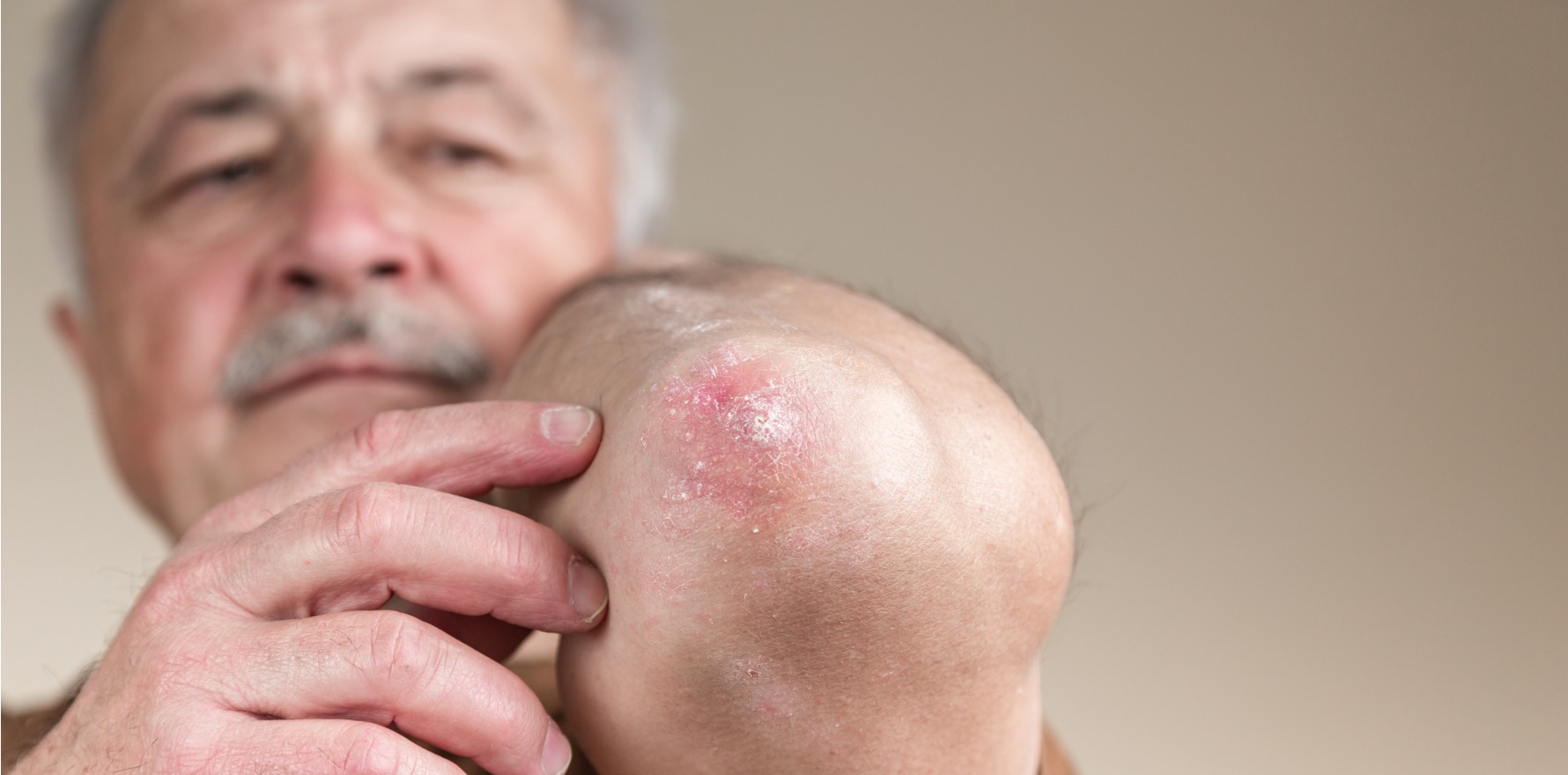
A new review provides helpful hints on the diagnosis and management of itch in the elderly.
Accurately diagnosing itch in elderly patients is more challenging compared to younger people, as pruritic eruptions can occur in the absence of any other obvious clinical symptoms.
A new review, published in The Journal of Allergy and Clinical Immunology, highlights how to identify and manage the leading causes of itch in elderly patients.
Dermatitis (38%), viral skin diseases (such as shingles, 6%), fungal skin diseases (such as athlete’s foot and ringworm, 4%) and psoriasis (3%) are the most common skin conditions in the elderly population, according to Global Burden of Disease data.
Among the elderly, itch is frequently characterised by xerosis (dry skin), neuropathic processes, neurological disorders (neuropathies, stroke) or poorly healing injuries.
Neuropathic processes can arise because of shingles infection, type 2 diabetes or central and peripheral nerve damage that occurs as part of the natural aging process.
As itch can have multiple individual or related causes, acquiring a thorough medical history is an important first step. Key recommendations from the review include inquiring about thyroid disorders, liver disease, neurological disorders, potential allergic reactions to medications or other household products and recent travel history.
While neurological disorders may not be front of mind in a patient presenting with itch, the authors point to a stroke or microinfarct in an itch-related area of the brain as a possible culprit.
Physical examination should focus on identifying evidence of systemic disease if no primary skin lesions are observed. Prurigo – itchy spots – are more common in the elderly and can present with nodules with or without erosions as secondary lesions.
A comprehensive range of laboratory tests can also be used to help determine the underlying cause of the itch, including complete blood counts (with liver function tests), HIV testing and hepatitis serologies. Chest radiographs can also be performed to check for underlying adenopathy. Skin biopsies are only recommended in patients with inflamed or diseased skin; they are less useful in patients with non-diseased or pruritic skin with severe scratch lesions.
Treatments for itch in the elderly are similar to those available for younger adults. However, comorbidities and other medical conditions need to be taken into account, not only when looking for the cause of the itch but also when it comes to selecting a treatment.
For example, determining whether comorbid dry skin and diabetic neuropathy are related or the result of separate causes. In addition, cyclosporine A, used to treat some pruritic inflammatory skin diseases, should not be used in patients with hypertension.
“We hypothesise that in elderly patients, the three pathophysiological routes of age-impacted immune system, epidermal barrier and peripheral/central nervous system interact with each other to collectively contribute to itch by modulating neuroinflammation that is mediated by various inflammatory mediators including neuropeptides, cytokines and chemokines,” the authors wrote.
The Journal of Allergy and Clinical Immunology 2023, online 21 May