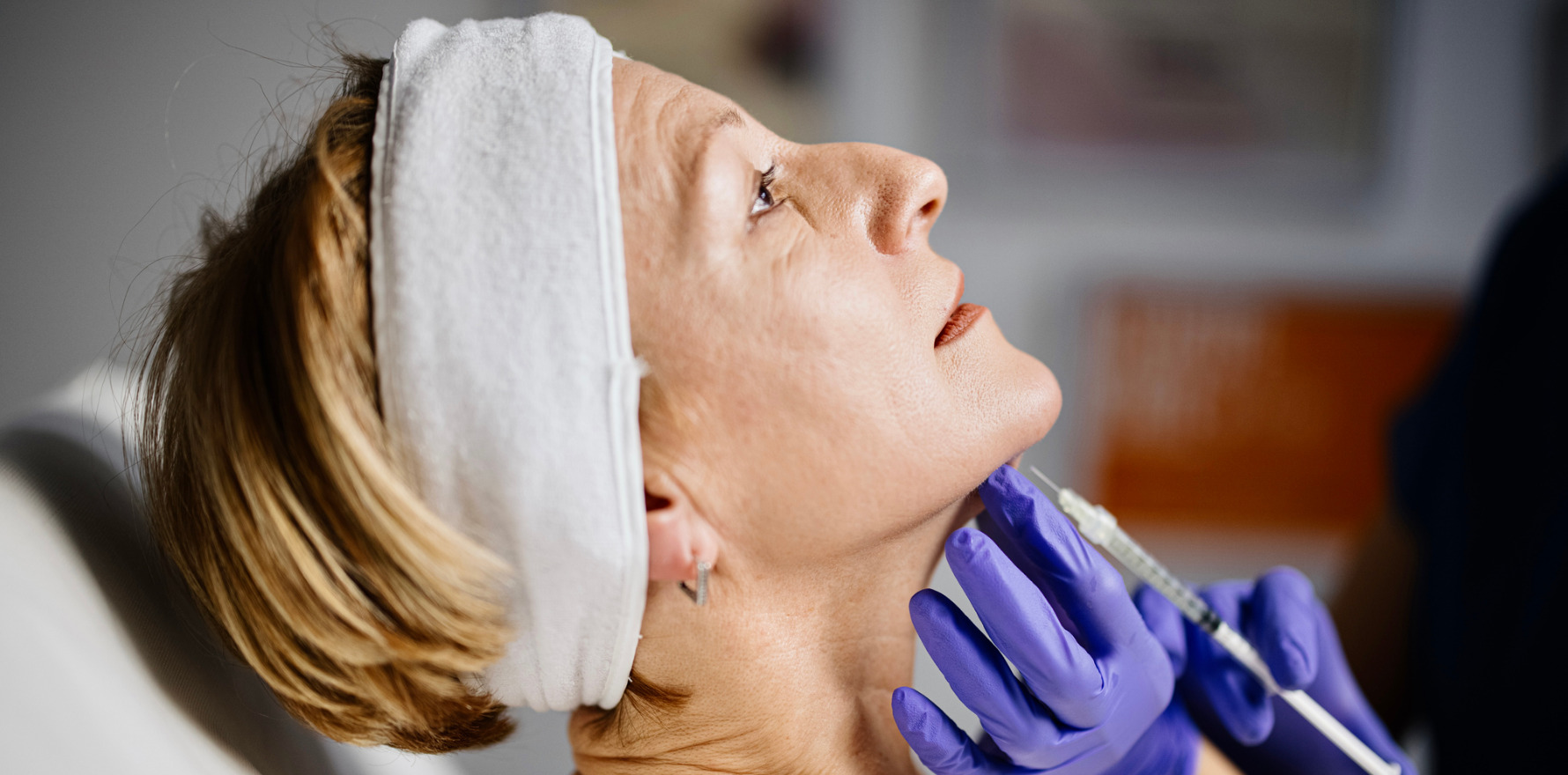
Following the crackdown on the cosmetic surgery sector, the new regulations will relate to both practice and advertising.
A year after an independent review into the cosmetic surgery industry, AHPRA and the MBA have announced new advertising and practice guidelines around non-surgical cosmetic procedures.
Non-surgical cosmetic procedures include treatments like botox and fillers, which can be performed by doctors, nurses and dentists.
According to AHPRA, “almost all” of the 16 reforms resulting from the review have been implemented.
Regulations relating to advertising will likely focus on before and after images, claims about expertise and qualifications of practitioners and the use of social media influencers, and will affirm the ban on the use of social media testimonials.
Practice guidelines will emphasise the adherence to informed consent and pre-procedure consultation – including patient suitability assessments – and may only allow for prescription-only cosmetic injectables.
AHPRA investigations over the past 18 months have revealed a lack of informed consent, minimal formal training provided to nurses around adverse reactions and a lack of consideration around mental health concerns.
“Getting these services is not like getting a haircut – these procedures come with risk,” said AHPRA CEO Martin Fletcher.
“We want to ensure the public knows what safe practice looks like, and that practitioners are doing everything necessary to keep the public safe.”
In the past year AHPRA received 179 formal complaints which have resulted in 14 doctors being either banned from practising cosmetic surgery or having “significant restrictions” in place while investigations continue. Twelve doctors have had restrictions placed on their registration after investigations.
In announcing the new moves AHPRA cited a number of case studies (all names have been changed):
- Yasmin, a patient with a history of mental illness, disclosed her history of body image issues to her doctor ahead of a series of filler injections. She also disclosed a history of 10 previous non-surgical cosmetic procedures she was unhappy with. Despite this, the doctor provided the filler injections as well as further treatments a month later. An investigation found the doctor failed to manage the patient’s mental health concerns, continued with treatment despite her body image issues and did not properly gain consent. Conditions are now on the doctor’s registration restricting practice.
- Jennifer was treated with dermal fillers by a registered nurse, despite having several known skin conditions that made the treatments inappropriate and dangerous. Following treatment, Jennifer had an adverse reaction to the treatment which required the fillers to be dissolved and steroid treatment to address the reaction. Additionally, the nurse inappropriately altered her treatment notes after a complaint was made. Following an investigation, the Board imposed conditions requiring the nurse to undertake formal education and provide a report reflecting on how they will change their practice in future.
- Carly suffered an infection in her cheek following a botched cosmetic thread lift procedure. Carly’s face become so infected she required surgery to firstly remove an abscess, and then surgery to restore her appearance. The doctor who led the thread lift was cautioned for failing to obtain informed consent, organise appropriate follow-up care, or use adequate infection control techniques. Another doctor who performed a similar procedure during the same training session was similarly cautioned.
The Cosmetic Surgery Hotline, which was launched on 5 September 2022 and allows patients, doctors, and consumers to informally flag concerns, has received 428 calls in the past year.
One doctor was found to have claimed that his procedures offered permanent results that would improve his patient’s self-confidence and used stock imagery rather than genuine before and after pictures.
Michael Fraser, co-director of patient advocacy group Operation Redress told the ABC that doctors “will often be more than happy to take your money and sell you procedures”.
“If you want to get procedures, get procedures, but you must be able to do so in a safe way. And you mustn’t have a doctor trying to upsell you or convince you that you have a problem that you didn’t know existed,” he said.
The Australasian College of Cosmetic Surgery and Medicine’s secretary and medical dean Dr Ronald Feiner told TMR that the ACCSM’s greatest concern is that “doctors and nurses aren’t working under the same roof” which he said, “doesn’t happen in any other medical field or hospital”.
“Unfortunately, a business model has emerged where a remote doctor prescribes for literally schools, if not hundreds of nurses,” he said.
“There is generally no doctor onsite so when a complication arises, they are on their own. They have to seek assistance in a remote session. And that’s not ideal.”
Dr Feiner said that Australia’s cosmetic surgery landscape was “approaching the situation in the UK where it’s completely out of control and is in crisis”.
“There are countries where new doctors can treat patients in any field of medicine with the assistance and co-operation of nurses, so Australia is heading down a terrible pathway.
“What we’re hoping is that a good sense of safety prevails … patients are not clients, they’re patients.”
Medical Board of Australia Chair Dr Anne Tonkin said: “We are already seeing a positive impact from strengthened practice and new advertising guidelines in the industry, and we are pleased that most practitioners have worked constructively with us towards these reforms.
“The endorsement for cosmetic surgery will also improve patient safety, by bringing in practice standards where there have been none.”