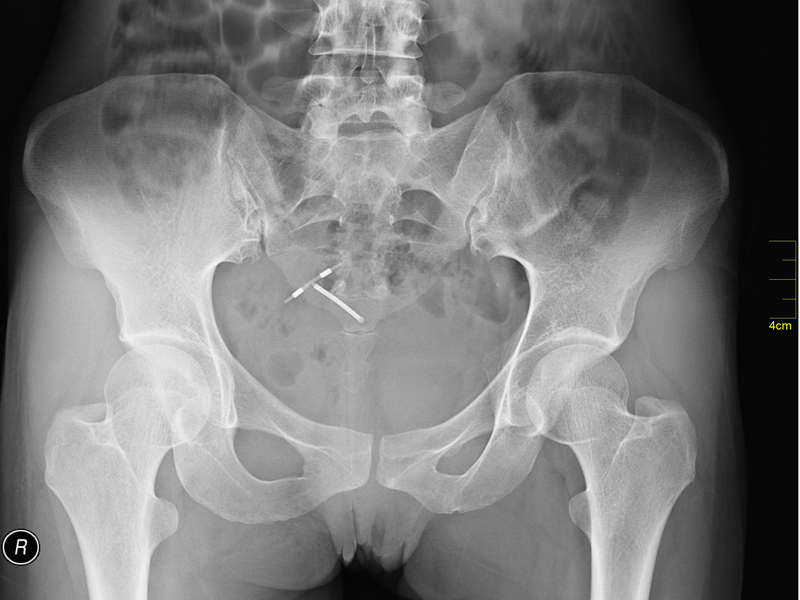
GPs that do not insert IUCDs still need to provide advice to women interested in this alternative
GPs that do not insert Intrauterine Contraceptive Devices still need to provide advice to women interested in this alternative.
“So often we think about contraception in terms of the pill,” says Dr Terri Foran, a sexual health physician at UNSW’s School of Women’s and Children’s Health.
“The very first thing for GPs is to remember to bring it up as an option.”
Dr Foran says that women are happy to know what else is out there even when they are satisfied with their current method of contraception.
“There are a lot of myths around IUCDs that really simply undeserved,” says Dr Foran.
“IUCDs are actually a very safe and very convenient form of contraception.”
Both copper and hormonal IUCDs can cause changes to bleeding patters. However, IUCDs are less likely to result in an unwanted pregnancy than the pill, which depends on the woman remembering to take each dose.
“I just wish our patients would see [IUCDs] more as a first choice rather than a last choice,” says Dr Foran.
In this video, Dr Foran discusses:
- What should GPs who don’t insert IUCDs tell patients who might be interested in having one before referring them?
- What are the problems regarding IUCDs?
- What are the advantages of hormonal IUCS?
- What are the non-contraceptive advantages of hormonal IUCDs?
- What about women who haven’t had surgery?
- What should patients expect immediately after insertion?
- Where can a GP learn to insert IUCDs?
- Take home messages?